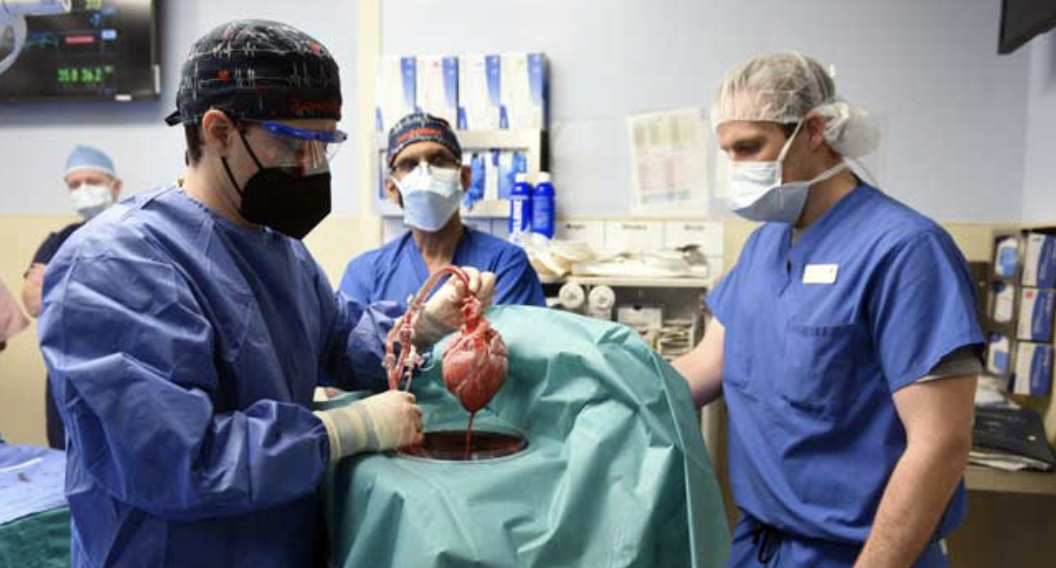
 Surgeons in the United States have successfully implanted a heart from a genetically modified pig into a 57-year-old man, a medical first that could one day help solve the chronic shortage of organ donations.
Surgeons in the United States have successfully implanted a heart from a genetically modified pig into a 57-year-old man, a medical first that could one day help solve the chronic shortage of organ donations.
The “historic” procedure took place on Friday, the University of Maryland Medical School said in a statement late Monday.
The nine-hour procedure was carried out at the University of Maryland Medical Center in Baltimore.
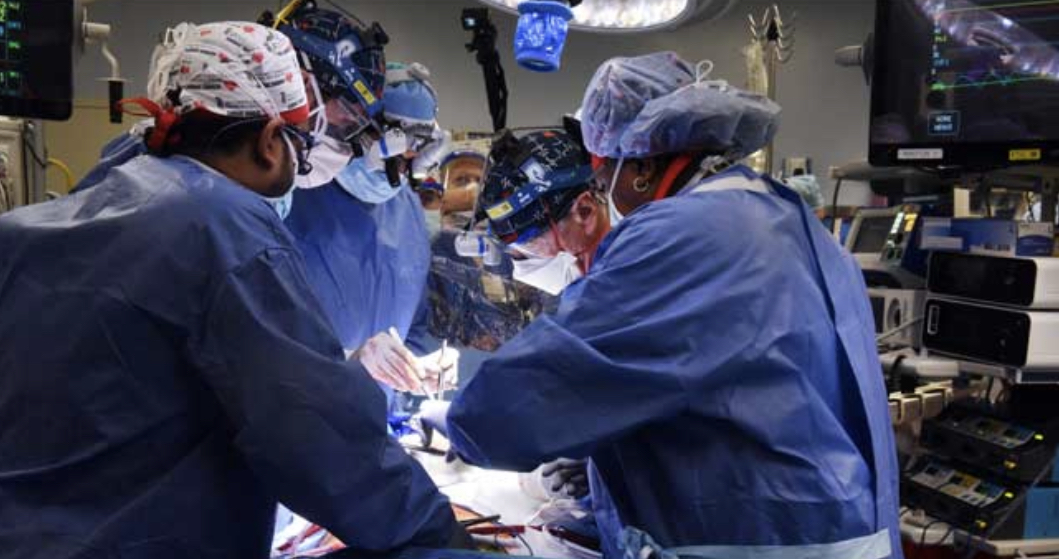
While the patient’s prognosis is far from certain, it represents a major milestone for animal-to-human transplantation.
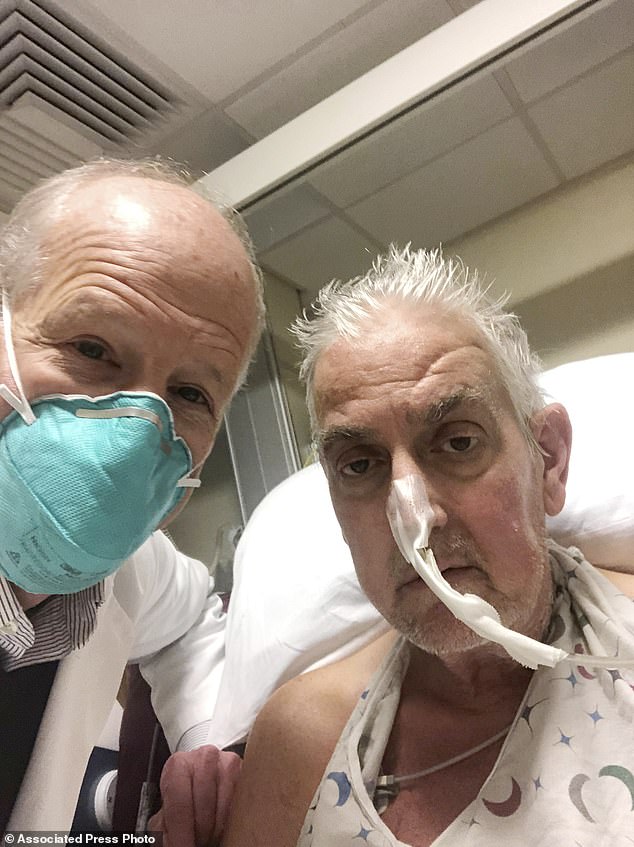
The patient, David Bennett, had been deemed ineligible for human transplant — a decision that is often taken when the recipient has very poor underlying health.
Bennett is now breathing on his own while still connected to a heart-lung machine to help his new heart pump blood around his body.

Experts say it is too soon to know if his body will fully accept the organ and the next few weeks will be critical as he is weaned off the machine.
However, if successful, it would mark a medical breakthrough and could save thousands of lives in the US alone each year.
Bennett, a labourer, knew there was no guarantee the operation would work but he was dying and ineligible for a human heart transplant.
A day before his surgery, Bennet said it was ‘either die or do this transplant‘, adding: ‘I want to live. I know it’s a shot in the dark, but it’s my last choice.’

He is now recovering and being carefully monitored to determine how the new organ performs.
Bennett, who has spent the last several months bedridden on a heart-lung bypass machine, added: “I look forward to getting out of bed after I recover.”
Food and Drug Administration granted emergency authorization for the surgery on New Year’s Eve, as a last-ditch effort for a patient who was unsuitable for a conventional transplant.
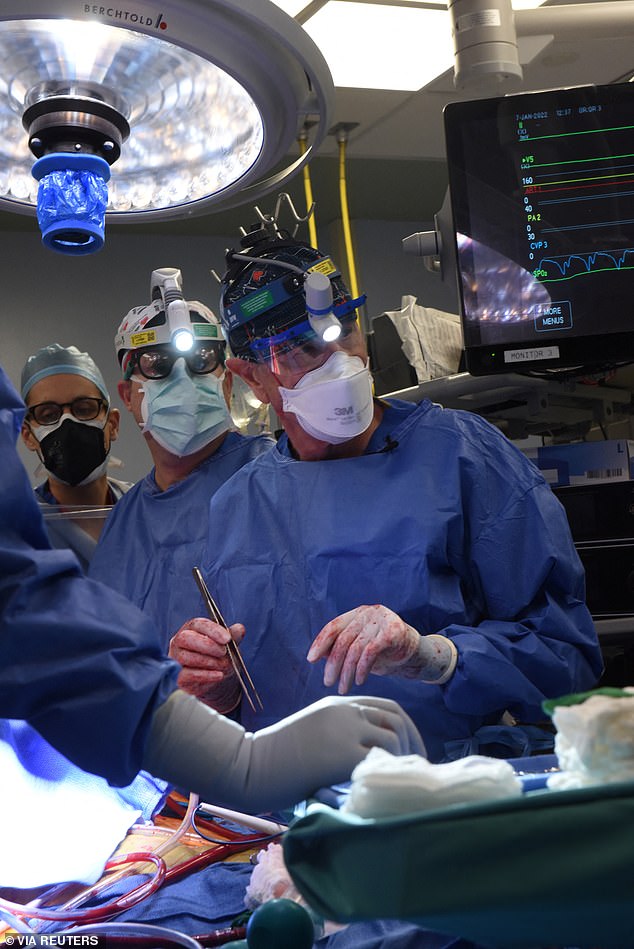
“This was a breakthrough surgery and brings us one step closer to solving the organ shortage crisis,” said Bartley Griffith, who surgically transplanted the pig heart.
He expressed;
We are proceeding cautiously, but we are also optimistic that this first-in-the-world surgery will provide an important new option for patients in the future.
On his part, Muhammad Mohiuddin, who co-founded the university’s cardiac xenotransplantation program, added the surgery was the culmination of years or research, involving pig-to-baboon transplants, with survival times that exceeded nine months.
He said;
The successful procedure provided valuable information to help the medical community improve this potentially life-saving method in future patients.
Bennett’s donor pig belonged to a herd that had undergone genetic editing procedures.
Three genes that would have led to the rejection of pig organs by humans were “knocked out,” as was a gene that would have led to excessive growth of pig heart tissue.
Six human genes responsible for human acceptance were inserted into the genome, for a total of 10 unique gene edits.
The editing was performed by Virginia-based biotech firm Revivicor, which also supplied the pig used in a breakthrough kidney transplant on a brain-dead patient in New York in October.
However, while that surgery was purely a proof-of-concept experiment, and the kidney was connected outside the patient’s body, the new surgery is intended to save a person’s life.
The donated organ was kept in an organ-preservation machine ahead of the surgery, and the team also used an experimental new drug made by Kiniksa Pharmaceuticals along with conventional anti-rejection drugs to suppress the immune system.
About 110,000 Americans are currently waiting for an organ transplant, and more than 6,000 patients die each year before getting one, according to official figures.
To meet demand, doctors have long been interested in so-called xenotransplantation, or cross-species organ donation, with experiments tracing back to the 17th century.
Early research focused on harvesting organs from primates — for example, a baboon heart was transplanted into a newborn known as “Baby Fae” in 1984, but she survived only 20 days.
Today, pig heart valves are widely used in humans, and pigskin is grafted on human burn victims.
Pigs make the ideal donors because of their size, their rapid growth and large litters, and the fact they are already raised as a food source.
Via AFP.

